The development of three-dimensional printing in neurosurgical departments across Europe: A five-year perspective

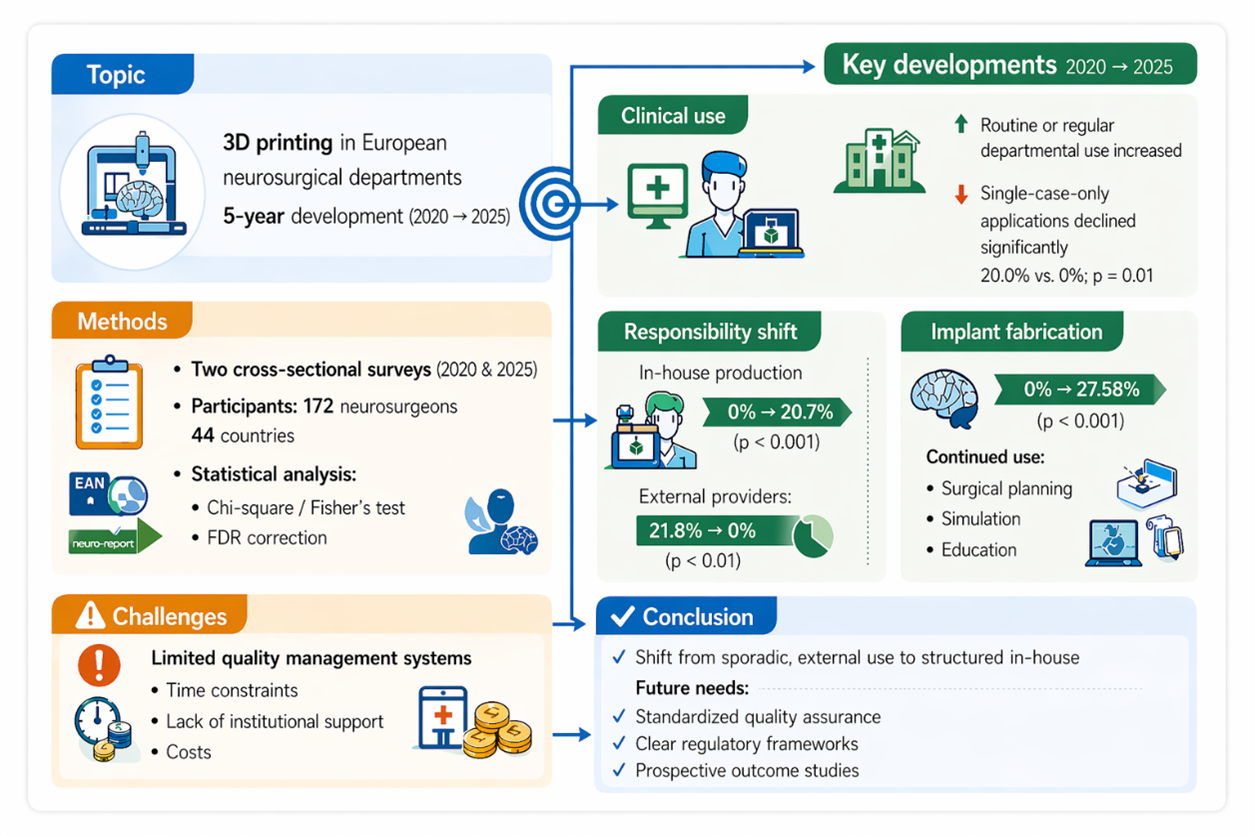
Three-dimensional (3D) printing has evolved into a valuable adjunct in neurosurgery, enabling patient-specific surgical planning, simulation, education, and implant fabrication. Although its technical feasibility and clinical utility are well documented, institutional integration and further development across European neurosurgical departments remain insufficiently defined. Two cross-sectional online surveys were conducted among European neurosurgeons in 2020 and 2025. The initial survey was distributed via the European Association of Neurosurgical Societies (EANS), while the follow-up survey was disseminated through national neurosurgical societies and direct re-contact of prior participants. A total of 172 completed questionnaires from 44 countries were included. Descriptive and comparative statistical analyses were performed using chi-square or Fisher’s exact tests with false discovery rate correction. Between 2020 and 2025, a significant maturation of 3D printing practices was observed. Routine or regular departmental use increased, whereas single-case-only applications declined significantly (20.0% vs. 0%; p = 0.01). Responsibility for printing shifted markedly toward in-house production: neurosurgeon-led printing increased from 0% to 20.68% (p < 0.001), while reliance on external providers decreased from 21.81% to 0% (p < 0.01). Implant fabrication emerged as a novel clinical application (0% vs. 27.58%; p < 0.001). Diversification of printing technologies and improved cost efficiency were reported; however, formal quality management procedures remained limited. Major barriers included restricted time resources, insufficient institutional support, and high costs. Over five years, 3D printing in European neurosurgery has transitioned from sporadic, externally dependent use toward structured, institutionally integrated workflows with expanding clinical applications. Standardized quality assurance, regulatory clarity, and high-quality prospective outcome studies are essential to further establish 3D printing as a routine clinical technology.
- Pucci JU, Christophe BR, Sisti JA, et al. Three-dimensional printing: technologies, applications, and limitations in neurosurgery. Biotechnol Adv. 2017;35(5):521-529. doi: 10.1016/j.biotechadv.2017.05.007
- McGurk M, Amis AA, Potamianos P, et al. Rapid prototyping techniques for anatomical modelling in medicine. Ann R Coll Surg Engl. 1997;79(3):169-174.
- Blohm JE, Salinas PA, Avila MJ, et al. Three-Dimensional Printing in Neurosurgery Residency Training: A Systematic Review of the Literature. World Neurosurg. 2022;161:111- 122. doi: 10.1016/j.wneu.2021.10.069
- D’Urso PS, Thompson RG, Atkinson RL, et al. Cerebrovascular biomodelling: a technical note. Surg Neurol. 1999;52(5):490-500. doi: 10.1016/s0090-3019(99)00143-3
- Dho YS, Lee D, Ha T, et al. Clinical application of patient-specific 3D printing brain tumor model production system for neurosurgery. Sci Rep. 2021;11(1):4627. doi: 10.1038/s41598-021-86546-y
- Duda S, Ivanyi P, Omar M, et al. Single-Session Surgical Intervention with Resection of a Primary Cranial Osteosarcoma and Cranioplasty using a 3D-Printed Craniotomy Template and Cranioplasty Molds. J Neurol Surg Rep. 2025;86(01):e8-e13. doi: 10.1055/a-2508-0868
- Duda S, Meyer L, Musienko E, et al. The Manufacturing of 3D Printed models for the Neurotraumatological Education of Military Surgeons. Mil Med. 2020;185(11-12):e2013-e2019. doi: 10.1093/milmed/usaa183
- Panesar SS, Magnetta M, Mukherjee D, et al. Patient-specific 3-dimensionally printed models for neurosurgical planning and education. Neurosurg Focus. 2019;47(6):E12. doi: 10.3171/2019.9.FOCUS19511
- Li S, Chen M, Wang H. Application of 3D Printing Positioning Technology in Parasagittal Meningioma Surgery: A Single-center Retrospective Study. World Neurosurg. 2024;192:e20- e26. doi: 10.1016/j.wneu.2024.06.134
- McGuire LS, Fuentes A, Alaraj A. Three-Dimensional Modeling in Training, Simulation, and Surgical Planning in Open Vascular and Endovascular Neurosurgery: A Systematic Review of the Literature. World Neurosurg. 2021;154:53-63. doi: 10.1016/j.wneu.2021.07.057
- Lan Q, Chen A, Zhang T, et al. Development of Three- Dimensional Printed Craniocerebral Models for Simulated Neurosurgery. World Neurosurg. 2016;91:434-442. doi: 10.1016/j.wneu.2016.04.069
- Lajczak PM, Jozwik K, Jaldin Torrico C. Current Applications of the Three-Dimensional Printing Technology in Neurosurgery: A Review. J Neurol Surg A Cent Eur Neurosurg. 2025;86(03):304-320. doi: 10.1055/a-2389-5207
- Randazzo M, Pisapia JM, Singh N, et al. 3D printing in neurosurgery: A systematic review. Surg Neurol Int. 2016;7(Suppl 34):S801-S809. doi: 10.4103/2152-7806.194059
- Tack P, Victor J, Gemmel P, et al. 3D-printing techniques in a medical setting: a systematic literature review. Biomed Eng Online. 2016;15(1):115. doi: 10.1186/s12938-016-0236-4
- Mery F, Aranda F, Mendez-Orellana C, et al. Reusable Low- Cost 3D Training Model for Aneurysm Clipping. World Neurosurg. 2021;147:29-36. doi: 10.1016/j.wneu.2020.11.136
- Piazza A, Corvino S, Colosso GQ, et al. 3-Dimensional Printed Model of the Temporal Bone for Neurosurgical Training. Oper Neurosurg. 2024;27(6):749-755. doi: 10.1227/ons.0000000000001213
- Robertson FC, Zygourakis CC, Wu JY, et al. Neurosurgical Resident Skill Development Using a Novel Simulator- Based Anterior Cervical Discectomy and Fusion Curriculum. World Neurosurg. 2025;201:124257. doi: 10.1016/j.wneu.2025.124257
- Ebel F, Schon S, Sharma N, et al. Clinical and patient-reported outcome after patient-specific 3D printer-assisted cranioplasty. Neurosurg Rev. 2023;46(1):115. doi: 10.1007/s10143-023-02000-9
- Nguyen B, Ashraf O, Richards R, et al. Cranioplasty Using Customized 3-Dimensional-Printed Titanium Implants: An International Collaboration Effort to Improve Neurosurgical Care. World Neurosurg. 2021;149:174-180. doi: 10.1016/j.wneu.2021.02.104
- Csamer L, Csernatony Z, Novak L, et al. Custom-made 3D printing-based cranioplasty using a silicone mould and PMMA. Sci Rep. 2023;13(1):11985. doi: 10.1038/s41598-023-38772-9
- Otero JJ, Vijverman A, Mommaerts MY. Use of fused deposit modeling for additive manufacturing in hospital facilities: European certification directives. J Craniomaxillofac Surg. 2017;45(9):1542-1546. doi: 10.1016/j.jcms.2017.06.018
- Pathak SM, Licata JP, Graves EKM, et al. Development of an adjustable patient-specific rigid guide to improve the accuracy of external ventricular catheter placement. J Neurosurg. 2024;141(4):1079-1087. doi: 10.3171/2024.2.JNS232137
- Bastawrous S, Wu L, Liacouras PC, et al. Establishing 3D Printing at the Point of Care: Basic Principles and Tools for Success. Radiographics. 2022;42(2):451-468. doi: 10.1148/rg.210113
- Bastawrous S, Wu L, Strzelecki B, et al. Establishing Quality and Safety in Hospital-based 3D Printing Programs: Patient-first Approach. Radiographics. 2021;41(4):1208-1229. doi: 10.1148/rg.2021200175
- Sag OM, Li X, Aman B, et al. Qualitative exploration of 3D printing in Swedish healthcare: perceived effects and barriers. BMC Health Serv Res. 2024;24(1):1455. doi: 10.1186/s12913-024-11975-0
- Daoud GE, Pezzutti DL, Dolatowski CJ, et al. Establishing a point-of-care additive manufacturing workflow for clinical use. J Mater Res. 2021;36(19):3761-3780. doi: 10.1557/s43578-021-00270-x
- Ganapathy A, Chen D, Elumalai A, et al. Guide for starting or optimizing a 3D printing clinical service. Methods. 2022;206:41-52. doi: 10.1016/j.ymeth.2022.08.003
- Hatamleh MM, Ong J, Hatamleh ZM, et al. Developing an In-house Interdisciplinary Three-Dimensional Service: Challenges, Benefits, and Innovative Health Care Solutions. J Craniofac Surg. 2018;29(7):1870-1875. doi: 10.1097/SCS.0000000000004743
- Awuah WA, Karkhanis S, Ben-Jaafar A, et al. Recent advances in 3D printing applications for CNS tumours. Eur J Med Res. 2025;30(1):142. doi: 10.1186/s40001-025-02483-w
- Sidabutar R, Yudha TW, Sutiono AB, et al. Low-cost and open-source three-dimensional (3D) printing in neurosurgery: A pilot experiment using direct drive modification to produce multi-material neuroanatomical models. Clin Neurol Neurosurg. 2023;228:107684. doi: 10.1016/j.clineuro.2023.107684
- Huang X, Fan N, Wang HJ, et al. Application of 3D printed model for planning the endoscopic endonasal transsphenoidal surgery. Sci Rep. 2021;11(1):5333. doi: 10.1038/s41598-021-84779-5
- Gomez-Feria J, Narros JL, Ciriza GG, et al. 3D Printing of Diffuse Low-Grade Gliomas Involving Eloquent Cortical Areas and Subcortical Functional Pathways: Technical Note. World Neurosurg. 2021;147:164-171.e4. doi: 10.1016/j.wneu.2020.12.082
- Waran V, Narayanan V, Karuppiah R, et al. Utility of multimaterial 3D printers in creating models with pathological entities to enhance the training experience of neurosurgeons. J Neurosurg. 2014;120(2):489-492. doi: 10.3171/2013.11.JNS131066
- Dhar S, Ahmad F, Deshpande A, et al. 3-Dimensional printing and bioprinting in neurological sciences: applications in surgery, imaging, tissue engineering, and pharmacology and therapeutics. J Mater Sci Mater Med. 2025;36(1):36. doi: 10.1007/s10856-025-06877-4
- Chepelev L, Wake N, Ryan J, et al. Radiological Society of North America (RSNA) 3D printing Special Interest Group (SIG): guidelines for medical 3D printing and appropriateness for clinical scenarios. 3D Print Med. 2018;4(1):8. doi: 10.1186/s41205-018-0030-y
- Langridge B, Momin S, Coumbe B, et al. Systematic Review of the Use of 3-Dimensional Printing in Surgical Teaching and Assessment. J Surg Educ. 2018;75(1):209-221. doi: 10.1016/j.jsurg.2017.06.033
- Vakharia VN, Vakharia NN, Hill CS. Review of 3-Dimensional Printing on Cranial Neurosurgery Simulation Training. World Neurosurg. 2016;88:188-198. doi: 10.1016/j.wneu.2015.12.031
- Jeising S, Liu S, Blaszczyk T, et al. Combined use of 3D printing and mixed reality technology for neurosurgical training: getting ready for brain surgery. Neurosurg Focus. 2024;56(1):E12. doi: 10.3171/2023.10.FOCUS23611
- Tong Y, Kaplan DJ, Spivak JM, et al. Three-dimensional printing in spine surgery: a review of current applications. Spine J. 2020;20(6):833-846. doi: 10.1016/j.spinee.2019.11.004
- Kim E, Vishwanath N, Foppiani J, et al. Barriers of Three- Dimensional Printing in Craniofacial Plastic Surgery Practice: A Pilot Study and Literature Review. J Craniofac Surg. 2024;35(4):1105-1109. doi: 10.1097/SCS.0000000000010271
- Ricles LM, Coburn JC, Di Prima M, et al. Regulating 3D-printed medical products. Sci Transl Med. 2018;10(461):eaan6521. doi: 10.1126/scitranslmed.aan6521
- Martelli N, Serrano C, van den Brink H, et al. Advantages and disadvantages of 3-dimensional printing in surgery: A systematic review. Surgery. 2016;159(6):1485-1500. doi: 10.1016/j.surg.2015.12.017
- Fuentes JM, Arrieta MP, Boronat T, et al. Effects of Steam Heat and Dry Heat Sterilization Processes on 3D Printed Commercial Polymers Printed by Fused Deposition Modeling. Polymers. 2022;14(5):855. doi: 10.3390/polym14050855
- St Clair-Glover M, Yue Z, Dottori M. 3D Printing for Neural Repair: Bridging the Gap in Regenerative Medicine. Adv Mater. 2025;37(36):2507590. doi: 10.1002/adma.202507590
- Sun B, Lian M, Han Y, et al. A 3D-Bioprinted dual growth factor-releasing intervertebral disc scaffold induces nucleus pulposus and annulus fibrosus reconstruction. Bioact Mater. 2021;6(1):179-190. doi: 10.1016/j.bioactmat.2020.06.022

