The impact on life in people with dissociative seizures or drug-resistant epilepsy

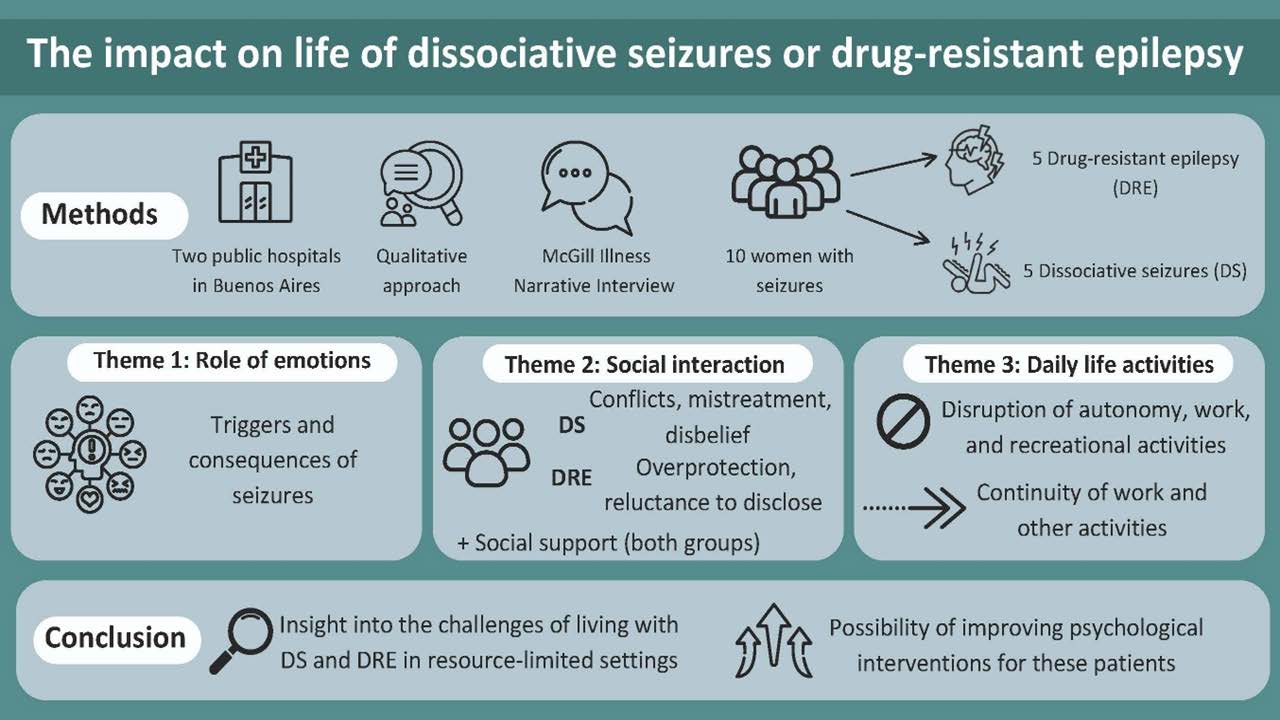
The aim of this study was to analyze and compare the impact on life in people with dissociative seizures (DS) and drug-resistant epilepsy (DRE). A qualitative approach was employed using the McGill Illness Narrative Interview, which was conducted and analyzed following thematic analysis principles. Ten women diagnosed with DS or DRE participated, all from underserved sectors in Argentina. Three major themes emerged from the interviews: (1) role of emotions (emotional experiences related to the disease, both preceding the seizure and as a consequence of them). Both groups reported unpleasant emotions as a consequence of seizures, such as fear, shame, and sadness. Emotional states, including stress and anxiety, were also described as seizure triggers in both conditions. (2) Impact on social interaction (the way in which the disease impacted on social relationships). Participants with DS experienced interpersonal conflicts, mistreatment, and disbelief more frequently than those with DRE, who reported a higher perception of overprotection and hesitancy to disclose their condition. Both groups acknowledged the importance of social support from family and friends. (3) Impact on daily life activities (the way in which people discontinued activities due to the disease or continued despite it). Seizures disrupted autonomy, work, and recreational activities, though some participants continued working despite limitations. These findings provide insight into the challenges of living with DS and DRE. A deeper understanding of these experiences can inform targeted interventions to improve the quality of life for these patient populations, particularly in resource-limited settings.
- Falco-Walter JJ, Scheffer IE, Fisher RS. The new definition and classification of seizures and epilepsy. Epilepsy Res. 2018;139:73-79. doi: 10.1016/j.eplepsyres.2017.11.015
- Fisher RS, Acevedo C, Arzimanoglou A, et al. ILAE official report: A practical clinical definition of epilepsy. Epilepsia. 2014;55(4):475-482. doi: 10.1111/epi.12550
- Fiest KM, Sauro KM, Wiebe S, et al. Prevalence and incidence of epilepsy: A systematic review and meta-analysis of international studies. Neurology. 2017;88(3):296-303. doi: 10.1212/WNL.0000000000003509
- Kalilani L, Sun X, Pelgrims B, Noack-Rink M, Villanueva V. The epidemiology of drug-resistant epilepsy: A systematic review and meta-analysis. Epilepsia. 2018;59(12):2179-2193. doi: 10.1111/epi.14596
- Kwan P, Arzimanoglou A, Berg AT, et al. Definition of drug resistant epilepsy: Consensus proposal by the ad hoc task force of the ILAE commission on therapeutic strategies. Epilepsia. 2010;51(6):1069-1077. doi: 10.1111/j.1528-1167.2009.02397.x
- Foley C, Kirkby A, Eccles FJ. A meta-ethnographic synthesis of the experiences of stigma amongst people with functional neurological disorder. Disabil Rehabil. 2022;46(1):1-12. doi: 10.1080/09638288.2022.2155714
- Popkirov S, Asadi-Pooya AA, Duncan R, et al. The aetiology of psychogenic non-epileptic seizures: Risk factors and comorbidities. Epileptic Disord. 2019;21(6):529-547. doi: 10.1684/epd.2019.1107
- Baslet G, Seshadri A, Bermeo-Ovalle A, Willment K, Myers L. Psychogenic non-epileptic seizures: An updated primer. Psychosomatics. 2016;57(1):1-17. doi: 10.1016/j.psym.2015.10.004
- Asadi-Pooya AA. Incidence and prevalence of psychogenic nonepileptic seizures (functional seizures): A systematic review and an analytical study. Int J Neurosci. 2021;133(6):598-603. doi: 10.1080/00207454.2021.1942870
- Jones B, Reuber M, Norman P. Correlates of health-related quality of life in adults with psychogenic nonepileptic seizures: A systematic review. Epilepsia. 2016;57(2):171-181. doi: 10.1111/epi.13268
- Taylor RS, Sander JW, Taylor RJ, Baker GA. Predictors of health-related quality of life and costs in adults with epilepsy: A systematic review. Epilepsia. 2011;52(12):2168-2180. doi: 10.1111/j.1528-1167.2011.03213.x
- Avalos JC, Silva BA, Tevés Echazu MF, Rosso B, Besocke AG, Del Carmen Garcia M. Quality of life in patients with epilepsy or psychogenic nonepileptic seizures and the contribution of psychiatric comorbidities. Epilepsy Behav. 2020;112:107447. doi: 10.1016/j.yebeh.2020.107447
- Rawlings GH, Brown I, Reuber M. Predictors of health-related quality of life in patients with epilepsy and psychogenic nonepileptic seizures. Epilepsy Behav. 2017;68:153-158. doi: 10.1016/j.yebeh.2016.10.035
- Salinsky M, Rutecki P, Parko K, et al. Health-related quality of life in veterans with epileptic and psychogenic nonepileptic seizures. Epilepsy Behav. 2019;94:72-77. doi: 10.1016/j.yebeh.2019.02.010
- Wolf LD, Hentz JG, Ziemba KS, et al. Quality of life in psychogenic nonepileptic seizures and epilepsy: The role of somatization and alexithymia. Epilepsy Behav. 2015;43:81-88. doi: 10.1016/j.yebeh.2014.12.010
- Rapport F, Clement C, Doel MA, Hutchings HA. Qualitative research and its methods in epilepsy: Contributing to an understanding of patients’ lived experiences of the disease. Epilepsy Behav. 2015;45:94-100. doi: 10.1016/j.yebeh.2015.01.040
- Epstein SA, Maurer CW, LaFaver K, Ameli R, Sinclair S, Hallett M. Insights into chronic functional movement disorders: The value of qualitative psychiatric interviews. Psychosomatics. 2016;57(6):566-575. doi: 10.1016/j.psym.2016.04.005
- Rawlings GH, Reuber M. What patients say about living with psychogenic nonepileptic seizures: A systematic synthesis of qualitative studies. Seizure. 2016;41:100-111. doi: 10.1016/j.seizure.2016.07.014
- Kerr C, Nixon A, Angalakuditi M. The impact of epilepsy on children and adult patients’ lives: Development of a conceptual model from qualitative literature. Seizure. 2011;20(10):764-774. doi: 10.1016/j.seizure.2011.07.007
- Keikelame MJ, Swartz L. “I wonder if I did not mess up….”: Shame and resistance among women with epilepsy in Cape Town, South Africa. Seizure. 2018;61:50-56. doi: 10.1016/j.seizure.2018.07.021
- Sarudiansky M, Lanzillotti AI, Oddo S, Kochen S, D’Alessio L, Pablo Korman G. Patients’ explanatory models about drug-resistant epilepsy in Argentina. A thematic analysis. Seizure. 2021;91:409-416. doi: 10.1016/j.seizure.2021.07.008
- Sarudiansky M, Korman GP, Scévola L, Oddo S, Kochen S, D’Alessio L. A life with seizures: Argentine patients’ perspectives about the impact of drug-resistant epilepsy on their lives. Seizure. 2018;63:52-61. doi: 10.1016/j.seizure.2018.10.008
- Sarudiansky M, Lanzillotti AI, Areco Pico MM, et al. What patients think about psychogenic nonepileptic seizures in Buenos Aires, Argentina: A qualitative approach. Seizure. 2017;51:14-21. doi: 10.1016/j.seizure.2017.07.004
- Rawlings GH, Brown I, Stone B, Reuber M. Written accounts of living with epilepsy or psychogenic nonepileptic seizures: A thematic comparison. Qual Health Res. 2018;28(6): 950-962. doi: 10.1177/1049732317748897
- Groleau D, Young A, Kirmayer LJ. The mcgill illness narrative interview (MINI): An interview schedule to elicit meanings and modes of reasoning related to illness experience. Transcult Psychiatry. 2006;43(4):671-691. doi: 10.1177/1363461506070796
- Hofmeijer I, Errazuriz C, Martel F. Spanish Version of McGill Illness Narrative Interview (MINI); 2013. Available from: https://www.mcgill.ca/tcpsych/files/tcpsych/mini_ spanish_0.pdf [Last accessed on 2025 Mar 25].
- Consalvo D, García MC, Giagante B. Guía para la realización de estudios de video-EEG de superficie [Guide for conducting surface video-EEG studies]. Rev Neurol Argent. 2009;1:50-55. [In Spanish]
- Baslet G, Bajestan SN, Aybek S, et al. Evidence-based practice for the clinical assessment of psychogenic nonepileptic seizures: A report from the American neuropsychiatric association committee on research. J Neuropsychiatry Clin Neurosci. 2021;33(1):27-42. doi: 10.1176/appi.neuropsych.19120354
- Wechsler D. Test De Inteligencia Para Adultos (WAIS) Manual [WAIS Adult Intelligence Test Manual]. Argentina: Paidós; 1995. [In Spanish]
- Braun V, Clarke V. Using thematic analysis in psychology. Qual Res Psychol. 2006;3:77-101. doi: 10.1191/1478088706qp063oa
- Patton DJ, Busch RM, Yee KM, Kubu CS, Gonzalez- Martinez J, Ford PJ. Hope language in patients undergoing epilepsy surgery. Epilepsy Behav. 2013;29(1):90-95. doi: 10.1016/j.yebeh.2013.07.005
- Rawlings GH, Brown I, Stone B, Reuber M. Written accounts of living with epilepsy: A thematic analysis. Epilepsy Behavior. 2017;72:63-70. doi: 10.1016/j.yebeh.2017.04.026
- Lang JD, Taylor DC, Kasper BS. Stress, seizures, and epilepsy: Patient narratives. Epilepsy Behav. 2018;80:163-172. doi: 10.1016/j.yebeh.2018.01.005
- Gelisse P, Genton P, Coubes P, Tang NP, Crespel A. Can emotional stress trigger the onset of epilepsy? Epilepsy Behav. 2015;48:15-20. doi: 10.1016/j.yebeh.2015.05.010
- McKee HR, Privitera MD. Stress as a seizure precipitant: Identification, associated factors, and treatment options. Seizure. 2017;44:21-26. doi: 10.1016/j.seizure.2016.12.009
- Goodman AM, Allendorfer JB, Heyse H, et al. Neural response to stress and perceived stress differ in patients with left temporal lobe epilepsy. Hum Brain Mapp. 2019;40(12):3415-3430. doi: 10.1002/hbm.24606
- Pick S, Goldstein LH, Perez DL, Nicholson TR. Emotional processing in functional neurological disorder: A review, biopsychosocial model and research agenda. J Neurol Neurosurg Psychiatry. 2019;90(6):704-711. doi: 10.1136/jnnp-2018-319201
- Sequeira AS, Silva B. A comparison among the prevalence of alexithymia in patients with psychogenic nonepileptic seizures, epilepsy, and the healthy population: A systematic review of the literature. Psychosomatics. 2019;60(3):238-245. doi: 10.1016/j.psym.2019.02.005
- Szaflarski JP, Allendorfer JB, Nenert R, et al. Facial emotion processing in patients with seizure disorders. Epilepsy Behav. 2018;79:193-204. doi: 10.1016/j.yebeh.2017.12.004
- Kret ME, De Gelder B. A review on sex differences in processing emotional signals. Neuropsychologia. 2012;50(7):1211-1221. doi: 10.1016/j.neuropsychologia.2011.12.022
- Cordaro DT, Sun R, Keltner D, Kamble S, Huddar N, McNeil G. Universals and cultural variations in 22 emotional expressions across five cultures. Emotion. 2018;18(1):75-93. doi: 10.1037/emo0000302
- World Health Organization. Psychologists Working in Mental Health Sector (Per 100,000). World Health Organization; 2019. Available from: https://www.who.int/data/gho/data/ indicators/indicator-details/GHO/psychologists-working-in-mental-health-sector-(per-100-000) [Last accessed on 2022 Feb 16].
- Elliott N, Pembroke S, Quirke M, Pender N, Higgins A. Disclosure strategies in adults with epilepsy when telling, “I have epilepsy”: The how2tell study. Epilepsia. 2019;60(10):2048-2059. doi: 10.1111/epi.16338
- Karakis I, Janocko NJ, Morton ML, et al. Stigma in psychogenic nonepileptic seizures. Epilepsy Behav. 2020;111:107269. doi: 10.1016/j.yebeh.2020.107269
- Robson C, Myers L, Pretorius C, Lian OS, Reuber M. Health related quality of life of people with non-epileptic seizures: The role of socio-demographic characteristics and stigma. Seizure. 2018;55:93-99. doi: 10.1016/j.seizure.2018.01.001
- Aydemir N. Overprotection and determinants of overprotection in adults with epilepsy. Seizure. 2020;79:14-19. doi: 10.1016/j.seizure.2020.04.006
- Gupta R, Garg D, Kumar N, et al. Psychiatric co-morbidities and factors associated with psychogenic non-epileptic seizures: A case-control study. Seizure. 2020;81:325-331. doi: 10.1016/j.seizure.2020.05.007
- Schönenberg M, Jusyte A, Höhnle N, et al. Theory of mind abilities in patients with psychogenic nonepileptic seizures. Epilepsy Behav. 2015;53:20-24. doi: 10.1016/j.yebeh.2015.09.036
- Gürsoy SC, Ergün S, Midi İ, Topçuoğlu V. Theory of mind and its relationship with alexithymia and quality of life in patients with psychogenic nonepileptic seizures: Comparisons with generalised epilepsy and healthy controls. Seizure. 2021;91(20):251-257. doi: 10.1016/j.seizure.2021.06.032
- American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders, Text Revision (DSM-5-TR). 5th ed. United States: American Psychiatric Association; 2022.
- Diprose W, Sundram F, Menkes D. Psychiatric comorbidity in psychogenic nonepileptic seizures compared with epilepsy. Epilepsy Behav. 2016;56:123-130. doi: 10.1016/j.yebeh.2015.12.037
- Vaidya-Mathur U, Myers L, Laban-Grant O, Lancman M, Lancman M, Jones J. Socialization characteristics in patients with psychogenic nonepileptic seizures (PNES). Epilepsy Behav. 2016;56:59-65. doi: 10.1016/j.yebeh.2015.12.032
- Pretorius C, Sparrow M. Life after being diagnosed with psychogenic non-epileptic seizures (PNES): A South African perspective. Seizure. 2015;30:32-41. doi: 10.1016/j.seizure.2015.05.008
- Leigh-Hunt N, Bagguley D, Bash K, et al. An overview of systematic reviews on the public health consequences of social isolation and loneliness. Public Health. 2017;152:157-171. doi: 10.1016/j.puhe.2017.07.035
- Rawlings GH, Brown I, Stone B, Reuber M. Written accounts of living with psychogenic nonepileptic seizures: A thematic analysis. Seizure. 2017;50:83-91. doi: 10.1016/j.seizure.2017.06.006
- Candela AG. Exploring the function of member checking. Qual Rep. 2019;24(3):619-628. doi: 10.46743/2160-3715/2019.3726

